Soft tissue surgery refers to any type of surgery for treatment of diseases which are not orthopaedic or neurologic.
As such, it encompasses surgery of most organs, the stomach, intestines, liver, kidneys, bladder, lungs, heart, as well as surgery of other soft parts of the body, including skin, muscle, and fat.
Our soft tissue surgeons are specialised in all these aspects of soft tissue surgery
Common Soft Tissue Surgeries
Here are some of the common soft tissue surgeries we perform if you would like to read more.
Thoracic Surgery
CHEST WALL MASSES
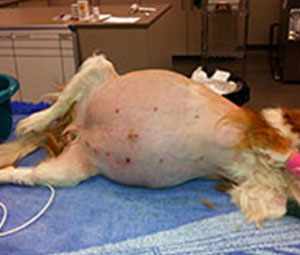
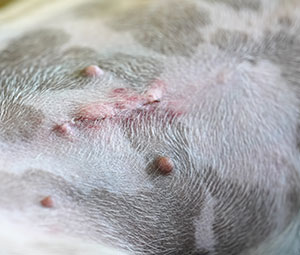
Masses or tumours of the chest wall come in many shapes, types and sizes. They can originate from the skin, soft tissue, muscle or bone and may be confined to a small area or be very extensive. Ideal management of these cases often requires a surgical biopsy to determine the cell type (eg infiltrative lipoma versus chondrosarcoma versus histiocytic sarcoma). A CT scan can determine the extent of the mass and facilitate surgical planning. Up to six ribs can be removed from the chest wall of some patients with full return of function, whereas in other cases the mass may be best treated by partial removal and then follow-up chemotherapy. Large mass resection may require reconstruction of the thoracic wall with techniques such as muscle and skin flaps, diaphragmatic advancement and prosthetic mesh insertion. Pre-operative surgical biopsies need to be taken in a way that does not compromise future resection of the entire mass. Several short term complications can arise from chest wall surgery, such as lung reperfusion injury, blood loss, pneumothorax and large seroma formation. Our skilled staff and excellent facilities are ready to manage these issues, however this means the patient may stay in hospital for 2-7 days after a major surgery.
LUNG TUMOURS and MASSES
Lung cancer is uncommon in dogs and rare in cats. Patients often present with a cough but few other symptoms, despite having a large area of lung lobe affected. Surgery can return quality of life for many months or cure the patient, depending on the location and type of the tumour.
Pulmonary carcinoma is the most common. Other causes of lung masses include grass seeds, abscesses, and granulomas. Dogs and cats have several lung lobes.
Depending on the tumour location, one or more lobes may need to be removed. Patients can return to excellent athletic function after lung lobectomy, once their bodies adjust to the change. Surgery to remove a lung lobe is planned well in advance (excepting emergency surgery for lung lobe torsion, which is performed as needed) and patients stay in hospital for 2-5 days post-operatively.The removed lung lobe is sent for histo-pathological analysis, and often for culture and sensitivity testing.
This helps us understand the underlying cause, and plan treatment to prevent relapse or recurrence.
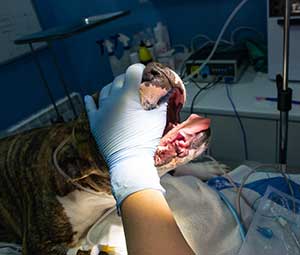
Chest wall mass surrounding lower ribcage, patient being clipped for biopsy of chest wall mass.

Chest wall mass surrounding lower ribcage


Soft Tissue Sarcomas
Soft tissue sarcomas include anaplastic sarcomas and histiocytic sarcomas and other undifferentiated growth of mesenchymal type cells. They can develop anywhere in the body, but are detected as a progressively enlarging semi-solid lump on the extremities (eg near the carpus, within the thigh or shoulder muscles, on the hock). They can grow at variable rates, and that rate can change. Liposarcomas- a fatty growth that behave in an aggressive way, have a similar appearance. The tumours are best removed early, before they interfere with ambulation. Because of their aggressive and invasive nature, wide margins are often required for successful removal. This may include up to 5 cm of normal tissue around the mass and one fascial plane or muscle layer beneath the lump. A combination of biopsy, ultrasound or CT scan may be used to determine the exact location and extent of the growth, to understand prognosis and aid surgical planning. Some masses respond better to a combination of chemotherapy and surgery, either before but usually after surgery.
CT scan showing Suzie’s soft tissue sarcoma in the serratusventralis, a muscle located between the shoulder blade and the rib cage. Suzie had a limp and a small lump protruding from her shoulder, but a large growth extending for 8 cm underneath the skin. It was successfully completely removed, thanks to the information gained from the CT scan.


Reproductive Tract/Urinary Tract Surgery
Incontinence
Young dogs may be incontinent due to a congenital anomaly, such as ectopic ureter or urethral sphincter mechanism incompetence (USMI). Ectopic ureters can be re-implanted into the bladder, improving or restoring continence. Prior to this surgery being performed, ultrasound, CT and/or cystoscopy is used to identify the size, location and health of the ureters and the kidneys they drain to determine prognosis and detect underlying infection. Occasionally we need to remove a deformed or damaged kidney, this is done at the same surgery. Concurrent or isolated USMI can be managed with medical therapy, or if unresponsive, colposuspension.
Trauma
Motor vehicle accidents can cause rupture of the bladder, tearing of the ureters or avulsion of a kidney. Leakage of the urine into the abdominal cavity is gradually toxic to the patient, and, can cause severe illness or even death over a 2-10 day period. Leaks and tears are detected using a combination of observation, blood and urine tests, and use of contrast dyes injected intravenously or via the urinary tract. These injuries are often associated with other injuries such as fractured pelvis, skin lacerations and rib fractures. Before the surgery, the patient must be stabilised to treat metabolic and electrolyte imbalances caused by urine accumulation. After repair of the leak or tear, the patient may require ongoing hospitalisation with an indwelling urinary catheter whilst the tract heals, for 2-7 days. Healing times depend on the severity of the injury.
Plastic & Reconstructive Techniques
8 ½ year old Border Collie with non-healing lesion on elbow after mass removal 5 months earlier.
Treatment via an axial pattern flap to cover right elbow. 35 days post-op.
Hindlimb shearing injury after debridement, granulation bed formation and final result after grafting and epithelialisation / contraction.

8 ½ year old Border Collie with non-healing lesion on elbow after mass removal 5 months earlier

Treatment via an axial pattern flap to cover right elbow. 35 days post-op
Liver Tumours
Liver tumours in dogs tend to be massive carcinomas, up to a basketball in size. This is not as bad as it sounds! These primary masses (occurring in the liver only) can be slow growing, and completely cured once resected. They are not simple surgeries however, as a result of a large and complex blood supply to the liver and surrounding organs. Use of automated staplers, special instruments for dissection, and sophisticated anaesthetic techniques are employed to minimise surgical time and risk. Up to 80% of the liver can be safely removed, and it will regenerate, however some central areas are essential to function and are irreplaceable. Pre-operative assessment of the patient is essential to determine prognosis (long term outcomes). This includes checking blood clotting, performing an abdominal ultrasound, and preferably a thoracic and abdominal CT scan. However the final decisions on surgical resection are made during surgery, and this is where having an experienced soft tissue surgeon becomes invaluable.
Jaundice in the eyes of a cat, abdominal skin of the dog.
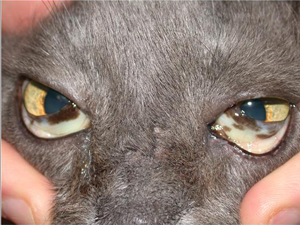
Jaundice in the eyes of a cat
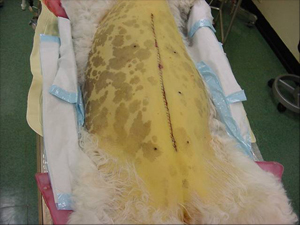
Abdominal skin of the dog
Laryngeal Paralysis
Laryngeal paralysis occurs when there is loss of function in the laryngeal muscles that normally open the larynx when an animal breathes in. The condition is caused by degeneration of certain nerves involved in normal breathing, and it results in airway obstruction causing noisy respiration. Laryngeal paralysis tends to affect mature age, large and giant breed dogs. Classically, these patients often present in late spring and early summer with progressive exercise intolerance or signs of heat stroke (constant panting, collapse, bright red mucous membranes, raspy breathing). Many dogs are affected by a degeneration of the nerve to the larynx (idiopathic). Some unluckier patients will have an underlying cancer of the larynx or mediastinal area, or hormonal or other medical disease that is altering nerve function. Patients are usually evaluated with full blood tests and chest xrays as well as examination of laryngeal function under a safe anaesthetic prior to surgery. Other tests are advised if clinically indicated. Treatment, which is effective in 90% of patients with idiopathic laryngeal paralysis, involves surgical abduction of one side of the larynx (“tie-back” procedure). This is a permanent alteration of the airway, allowing better air flow into the lungs. Patients recover quickly, but must wear a chest harness instead of a neck lead after surgery. They are fed slowly, to decrease the (low) risk of aspiration pneumonia. Although many patients are 12-14 years of age when they develop this condition, age is not a disease or reason not to proceed. We discuss carefully with the owners what quality of life their pet currently enjoys and what they can expect after the surgery has been performed.

Hernia Surgery
Hernias can result as a congenital deformity, secondary to trauma or chronic straining. Some hernias require emergency surgery due to strangulation of organs. Hernias that are successfully treated include: Hiatal hernia- when the stomach slides through the diaphragm, into the chest within or next to the oesophagus. Most commonly seen in English Bulldogs, French bulldogs and Shar Peis. This is treated with oesophagopexy, gastropexy and phrenicoplasty. Diaphragmatic hernia: most often seen in cats and dogs after a motor vehicle accident. Sometimes it is not detected until months after the accident occurred. The stomach, liver, spleen and intestines may slide into the chest cavity, interfering with lung function. These organs are replaced in the abdomen (or removed if needed) and the tear(s) in the diaphragm closed. Inguinal hernia, scrotal hernal, umbilical hernia: displaced organs are repositioned and the defects safely closed. Perineal hernia: Thorough investigation into the underlying cause of a perineal hernia is essential. Breeds such as Border Collie have an inherent weakness of the pelvic diaphragm muscles. Many other breeds develop perineal hernia as a result of straining to defecate or urinate. The common underlying causes of this include prostatic disease, such as benign prostatic hyperplasia, colonic or rectal disease such as IBD, polyps or carcinoma, or cystitis, due to calculi formation with concurrent infection. Less common causes include prostatic or rectal adenocarcinoma, sarcoma of the pelvic canal, megacolon and narrowed pelvic canal due to previous fracture. These problems are best detected using clinical examination, and/or radiographs, ultrasound, CT or colonoscopy and FNA of relevant organs. Each case must be assessed on its own merits. Surgery can be done on one side or both at the same time, once again depending on the case. Hernia repair may entail movement of the internal obturator, superficial gluteal, semitendinosus muscle or insertion of a prosthetic mesh.
Foreign Body Removal
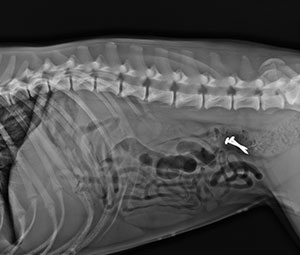
A common surgery we perform is to remove foreign bodies from the gastro-intestinal tract of dogs and cats that eat materials such as parts of stuffed toys, scouring pads, carpet, plastic bags, string, sewing needles, bones, socks and underwear! These items can get stuck in the oesophagus (95% of these can be retrieved by endoscopy), stomach, or intestines (often at the ileo-caecal valve). Other foreign materials, such as grass seeds and sticks, can be accidently swallowed, inhaled or penetrate the feet and skin and work their way to remote sites. One of the most common places for migrating grass seeds to go is under the lumbar spine, forming a small abscess close to the aorta. These are best located using ultrasound or a CT scan, and removed with extreme care by our soft tissue surgeon. Animals can suffer recurring fever, pain, draining sinuses and debilitation until the foreign material is completely removed. Foreign bodies lodged in the gastrointestinal tract can lead to life-threatening infections and eventual death if not treated.
Stockings from the stomach of a dog.

Stockings from the stomach of a dog
Ear Surgery
Total Ear Canal Ablation and Bulla Osteotomy (TECABO)
TECABO is used to treat chronic inflammation or cancer. Chronic inflammation as a result of life-long allergies or congenitally stenotic ear canals leads to pain and secondary thickening and infection of the ear pinna and canal. The entire canal can be safely removed, alleviating symptoms. The tympanic bulla (bony part of the skull that the ear canal originates from) must be opened up as well, to facilitate drainage of infection and debridement of the origin of the canal epithelium. Hearing is often impaired pre-operatively, but is not worsened by the procedure.
Pinna surgery
Pinna surgery is performed to remove sarcomas, treat lacerations and aural haematomas, if required. White eared cats with solar damage causing squamous cell carcinoma can have the majority of the pinna removed to manage this disease. Skin flaps (movement of skin including a vascular pedicle) can be utilised to manage skin tension/tissue defects if radical surgery is needed.



Cardiac Surgery
PERICARDECTOMY
Subtotal pericardectomy involves removal of the lower 2/3 of the pericardium (heart sac) to allow fluid to drain into the thoracic (chest) cavity. The fluid may be present because of cancer (often mesothelioma, occasionally haemangiosarcoma) or a condition called idiopathic pericardial effusion, where no known cause can be detected, but the problem is recurring and life-threatening. If excessive fluid is trapped within the pericardial sac, the heart cannot expand to pump blood, and rapidly fails.
Subtotal pericardectomy can be performed with surgical access between the ribs in most situations. If there is restrictive pericarditis, where the heart sac has become fibrotic from chronic inflammation, or a tumour mass must be accessed from a particular direction (eg left heart base) the surgical approach may be altered. Restrictive pericarditis is more likely when the fluid has been drained several times via needle already (pericardiocentesis). The risks of cardiac surgery include arrhythmias, blood loss, nerve injury and pleural effusion. Consultation with the surgeon occurs before every case goes to surgery, and is essential for understanding the risks and long term outcomes expected for this surgery. Radiograph of a 70 kg canine patient after pericardectomy to treat congential pericardial cysts. The sternum has been closed with wire.
PATENT DUCTUS ARTERIOSUS
Patent ductus arteriosus (PDA) is a congenital defect seen in all dogs but is more common in Border Collies, German Shepherds, and other purebred dogs.It tends to affect females more than males. It is often detected at puppy vaccinations and should be treated at an early age, preferably before 4-5 months of age. The longer it is left untreated, the more secondary degenerative changes occur in the heart muscle and valves. Diagnosis is confirmed by echocardiogram (ultrasound of the heart) which shows the heart vessel (ductus) which failed to close at birth.
Surgery has a very high success rate (99% are permanently cured). Surgery involves opening the chest between the ribs to access the heart. The ductus is dissected free and tied off (ligated). Patients recover very rapidly and must be confined after surgery to ensure they rest- as puppies they just want to play and play with their new-found energy!


Brachycephalic Obstructive Syndrome
Brachycephalic obstructive syndrome (BOS) is a condition affecting Bulldogs, Pugs, Cavalier King Charles Spaniels and other Brachycephalic breeds with very short noses and flat faces. These patients are extraordinarily cute, but have limited respiratory capacity as a result of narrowed nostrils, elongated soft palate, extra-large tongues and narrow tracheas. Secondary changes develop in the soft tissues of the throat/pharynx, larynx, and trachea resulting in collapse of the airways, incredible snoring and breathing noises, and eventual exercise intolerance, heat stroke and collapse. The condition can be improved by surgically trimming the soft palate to a safe length, removing the abnormal tissue, and opening up the nostrils. In severe conditions, the trachea can be supported, either internally or externally. Medications and dietary management of this condition are also essential and can help to dramatically improve symptoms. Young brachycephalic patients (age 6+ months) can benefit from early surgery to delay or halt progression of the symptoms.


Abdominal Surgery
Stomach, intestines, liver, spleen, kidneys, adrenal glands, the list goes on. A lot of vital organs exist within the abdominal cavity, and illness in one can upset the balance in the rest of the system. Whether the original problem is trauma (eg hit by car) or cancer or something the patient ate (such as a cooked bone), determines what surgery is required. Sometimes the problem is obvious, sometimes a series of tests such as blood analysis, x-rays, ultrasound and CT scan are required to fully understand the extent of the problem and the patient’s prognosis. We are fully equipped to deal with all manner of abdominal surgery.
Examples of diseases we treat include:
- Liver: mass removal, biopsy for disease, portosystemic shunts, liver lobe torsion
- Gall bladder: removal, diversion, flushing and stenting of the common bile duct
- Spleen: partial or complete splenectomy for mass removal, splenic torsion
- Stomach: gastric torsion, gastric dilation, mass removal, treatment of pyloric stenosis, preventative gastropexy, foreign body removal, G-tube placement, duodenal bypass
- Intestines: removal of obstructive foreign bodies and masses, mesenteric torsion, intussusception, megacolon, disease within the colon and rectum, duodenal perforation, peritonitis
- Kidneys: nephrectomy, opening of the renal pelvis to remove stones, biopsy
- Ureters: torn, transected or ligated ureters re-anastomosis, ectopic ureter re-implantation
- Bladder: removal of stones, tumours, ruptured bladder, urethral sphincter mechanism incompetence, urethrotomy
- Adrenals: mass removal, including those with caval invasion, if required and appropriate
- Pancreas: biopsy, partial removal, insulinoma removal Ovaries/uterus: caesarean, spey, uterine torsion, tumour removal
Not on the list? Please ask, these are examples.